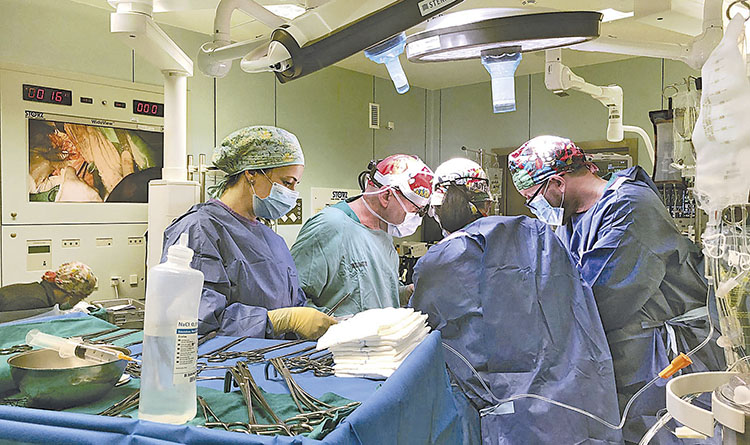
With 48.3 organ donors per million population in 2018, Spain is very near to reaching the goal of 50 donors per million, along with the aim of performing 5,500 transplants per year by 2022. This is double the average for the European Union and higher than the United States (32.8). These figures are testament to the success of a system that was first developed 30 years ago, when the country barely had 15 donors per million population.
The WHO estimates that 5-10% of transplants involve illegal organ trafficking: in order to combat this trade, Spain has successfully submitted a number of resolutions for approval by the United Nations
Today, the World Health Organisation (WHO), the United Nations and the Council of Europe all promote the adoption of the Spanish model in other countries as an alternative to organ trafficking and “transplant tourism”. (In Spain, only Spanish citizens or legally resident foreigners can receive transplants.) Within the European Union, the model has been implemented –either fully or partially– in Croatia, Italy, France, Portugal, the Czech Republic, Hungary and Austria; while in the rest of the world, countries such as Australia and Canada have incorporated elements of the system. Additionally, for the last 15 years Spain has operated a training and advisory network in Latin America, where both donation and transplantation rates have increased in every country.
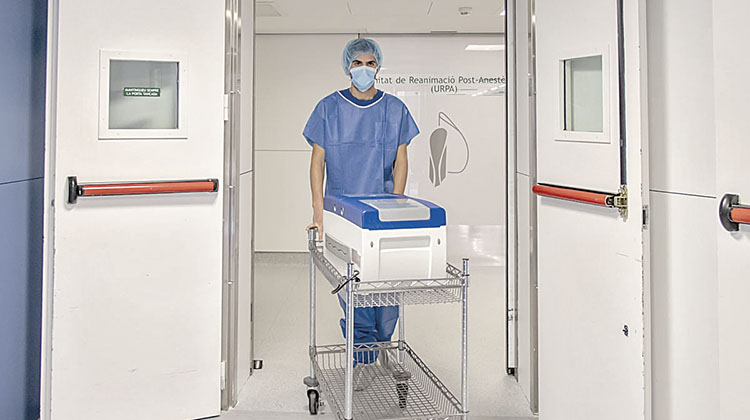
Since 2006, Spain has worked with the WHO to manage the International Registry of Organ Donation and Transplantation, according to which around two million people per year require a transplant, although just 145,000 are performed. / PHOTO_HOSPITAL CLÍNIC BARNA (A. CREUS y Á. GARCÍA)
The Spanish model began to take shape in 1989, with the passing of a law based on the principles of complete anonymity and altruism on the part of the donor and their family, full respect for their wishes, and absolute equality in the distribution of available organs to transplant patients, in accordance with medical criteria. Additionally, so-called “encephalic death” was declared the scientific, legal and ethical equivalent of “traditional” death. Encephalic death also has to be diagnosed by a separate medical team that is not involved with the transplantation.



A race against time
The law, which was implemented in the years that followed, also established the creation of the National Transplant Organisation (Organización Nacional de Trasplantes, ONT), part of the Ministry of Health. Since then, this body has been responsible for managing and coordinating a dual process, which starts by identifying potential donors in hospitals (via a coordinator or dedicated team, depending on the size of the hospital), obtaining the family’s consent, and commencing the urgent process of extracting, storing and transporting the organs to the hospital where the transplant will take place. While this is going on, compatible recipients are located and transferred to the hospital. It is a race against time, as the window before the organs start to deteriorate, known as ischemia time, is just a few hours long. The shortest window, for hearts and lungs, is three to four hours, and a little longer for kidneys (the most frequently transplanted organ). For this reason, and although medical considerations and the severity of the patient’s case are always the predominant criteria, geography is also taken into account in order to minimise the distance travelled and prevent the organs from deteriorating. The exception is so-called “urgency level zero”, when a patient is so critical they have absolute priority on a nationwide basis.

Tribute to all transplant professionals by the city of Madrid. / PHOTO_MADRID CITY COUNCIL
Although, according to the ONT, 10% of patients still die while awaiting a transplant, in the last 30 years more than 51,000 Spaniards have donated organs –including over 5,000 living donors of kidneys or livers– and more than 116,000 transplants have been performed.
According to the Ministry of Health, today nine out of ten Spanish families consent to the donation of organs, each of which literally adds years (the ONT estimates between 31 and 56 years, depending on the number of organs) to the lives of the patients that receive them.
Key features of the Spanish transplantation model
- The hospital’s transplant coordinator (or coordination team), usually an intensive care specialist, manages immediate donations.
- Potential donors are identified in hospitals (ICU, A&E, hospitalisations) as well as outside (donation after circulatory death or asystole) and donors over 65 years of age are assessed.
- The system is publicly funded and hospitals are reimbursed for the costs of extraction and transplantation, which enables smaller clinics to take part. For the patient, the process is entirely free of charge.
- Continuous training of healthcare professionals.
- The ONT acts as a service and coordination agency between different administrations.
- Legislation to define and regulate the entire process.
- Continuous information and awareness-raising activities involving the media, in order to increase knowledge among the population.
Source: ONT